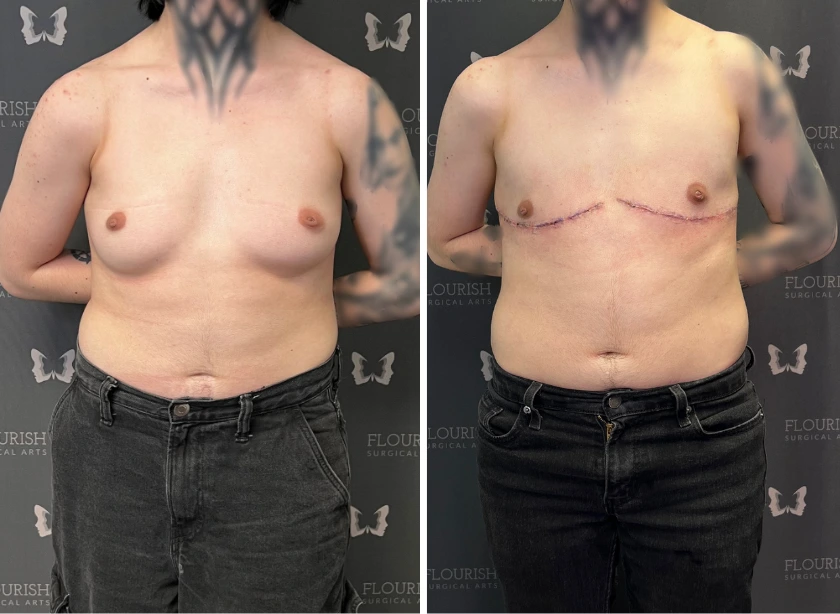
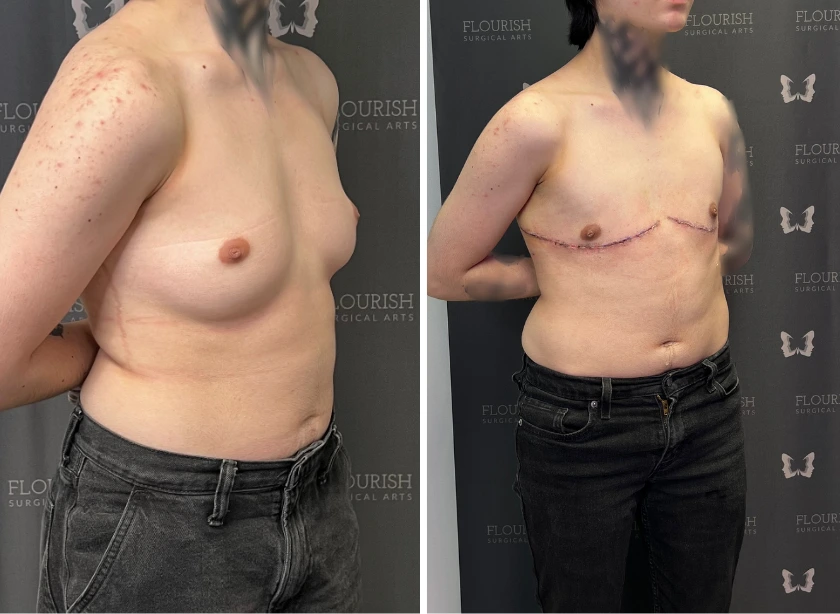
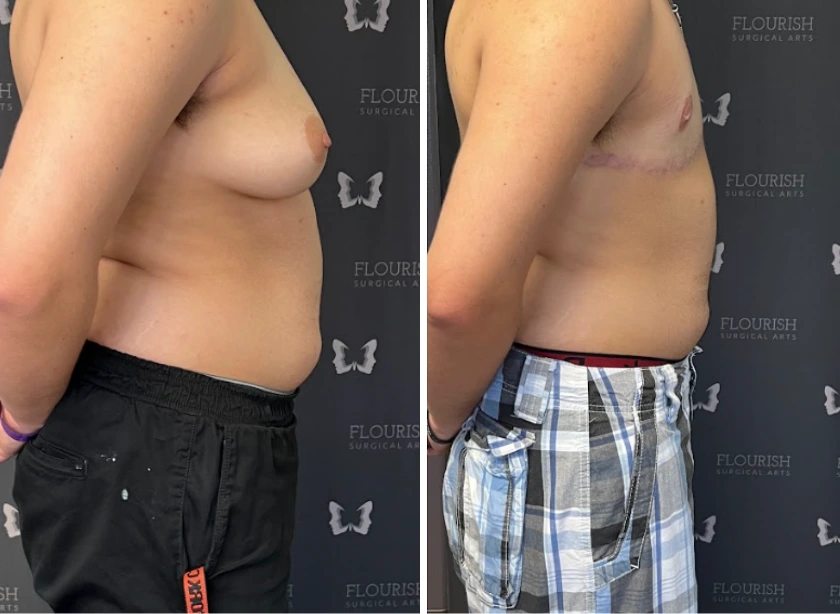
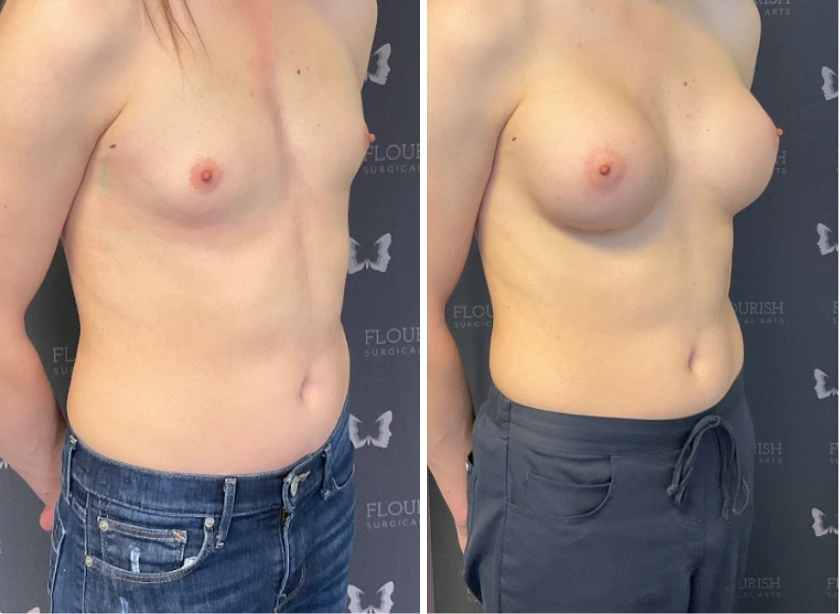
Top Surgery Recovery Timeline: What to Expect Week-by-Week (FTM and MTF)?
Top surgery is one of the most meaningful steps many transgender individuals take in their gender-affirming journey – and knowing what to expect afterward can make the experience far less daunting. Most patients are surprised to learn that the initial recovery period lasts about six weeks, with full healing taking anywhere from three to six months. While everyone’s body is different, the top surgery recovery timeline follows a fairly predictable pattern: the first two weeks are the most physically demanding, weeks three through six involve a gradual return to daily life, and the months that follow are mostly about scar maturation and final results coming into view.

Understanding the Overall Recovery Process
Understanding the Overall Recovery Process
Whether you’re undergoing FTM (female-to-male) chest masculinization or MTF (male-to-female) breast augmentation, top surgery recovery shares many common threads. Both procedures require rest, restricted movement, and careful wound monitoring. That said, there are key differences.
FTM top surgery – which typically involves double incision, periareolar, or keyhole techniques – tends to involve more extensive tissue removal, drainage tubes, and in many cases, free nipple grafts.
MTF top surgery involves breast implant placement, which carries its own set of positioning restrictions and healing considerations.
Understanding what’s normal versus what warrants a call to your surgeon is one of the most empowering things you can do before going under the knife.
Your First Week After Surgery
The first week is the hardest – there’s no sugarcoating it. You’ll wake up from anesthesia feeling groggy, tight, and sore. A compression vest or surgical bra will be secured firmly around your chest, and depending on your procedure, you may have one or two drainage tubes collecting fluid from the surgical site.
Here’s what most patients experience during days one through seven:
Pain and tightness: Manageable with prescribed pain medication; transitions to over-the-counter options by day three or four for many patients
Drains (FTM patients): These are usually removed within five to seven days once output drops below a certain threshold – your surgeon will set that number
Limited arm movement: Reaching above shoulder height is off-limits; even simple tasks like washing your hair will require help
Fatigue: Your body is doing enormous work internally; sleeping more than usual is completely expected
Swelling and bruising: Both peak around days three to five before gradually subsiding
You’ll need a dedicated caregiver for at least the first three to five days. Arrange this before your surgery date, and don’t underestimate how much you’ll need them. Set up a recovery station with everything within arm’s reach: medications, water, snacks, a phone charger, and entertainment.
Further Recovery
Weeks 2-3: Turning the Corner
By the start of week two, most patients begin to feel more like themselves. Pain becomes more manageable, and drains are typically removed (for FTM patients). You may still feel emotionally raw, and this is completely normal.
Swelling remains significant but starts to visibly decrease
You can likely shower (with surgical site protection) by day seven to ten, pending surgeon approval
Short, gentle walks are encouraged to promote circulation
Driving is still off-limits if you’re on prescription pain medication
Week three brings more noticeable improvement. Many patients transition fully to over-the-counter pain relief and begin to feel restless – which is a good sign, though it can also lead to overdoing it. Resist the urge.
Weeks 4-6: Building Momentum
This stretch is where most patients feel a meaningful shift. Incisions are knitting together, swelling is continuing to resolve, and the emotional relief of seeing early results starts to set in.
MTF patients may notice their implants sitting high on the chest during this period – this is completely normal and part of the “dropping and fluffing” process that takes several months. FTM patients will begin to see their chest contour
Caring for Nipple Grafts During Recovery
For FTM patients who undergo double incision top surgery, nipple grafts deserve special attention. Free nipple grafts are removed, resized, and repositioned on the chest, and they undergo a distinct healing process that can alarm patients who aren’t prepared for it.
In the first week, the grafts are covered with bolster dressings that apply pressure to promote integration with the underlying tissue. When those dressings come off (usually around day five to seven), the nipples may appear dark, crusty, or discolored. This can be startling, but it’s part of normal graft healing.
Weeks 1-2: Bolster removal; grafts may look dark brown or almost black
Weeks 3-4: Scabbing and peeling; the outer layer sloughs off to reveal new tissue underneath
Weeks 6-12: Color and sensation gradually return for many patients, though full sensation can take up to a year, or may be permanently reduced
Never pick at graft scabbing, and keep the area clean and moisturized only as your surgeon instructs.
Post-Op Care Essentials That Make a Real Difference
Strong post-op care is what separates a smooth recovery from a complicated one. Your surgical team will provide specific instructions, but some universally important principles apply across both FTM and MTF top surgery.
Scar management typically begins around six weeks post-op once incisions are fully closed. Silicone sheets or gels, applied consistently and combined with massage, are considered the gold standard for minimizing scar appearance. Sun protection over scars is non-negotiable for at least a year, as UV exposure can permanently darken them.
Sleep position matters more than most patients expect. Sleeping on your back, slightly elevated, reduces swelling and protects your incisions. For MTF patients with implants, this position also prevents implant displacement during the critical early weeks.
Nutrition plays an underrated role, too. Protein, vitamin C, and zinc all support tissue repair. Avoid alcohol and smoking both before and after surgery, as they significantly impair healing at the cellular level.
Surgery Recovery Tips to Promote Healing Faster
While there’s no way to fast-track biology, there are smart strategies to support your body’s natural process:
Follow your compression garment schedule exactly – it controls swelling and supports tissue remodeling
Don’t skip follow-up appointments, even if you feel fine; internal healing isn’t visible from the outside
Hydrate consistently – dehydration slows healing and worsens fatigue
Prepare your mental health support – top surgery is joyful, but the recovery period can also surface unexpected emotions; having a therapist or support community in place matters
Ask questions freely – no concern is too small to bring to your surgeon’s team
Returning to Normal Activities
Returning to normal activities is a gradual process, not a switch that flips at the six-week mark. Most surgeons use a tiered timeline:
Light walking is encouraged from week one.
Desk work and light daily tasks typically resume around weeks two to three.
More vigorous activity – including lifting anything over ten pounds – is usually cleared around weeks four to six.
High-impact exercise, contact sports, and heavy gym work are generally off-limits until at least three months post-op, sometimes longer for MTF patients with implants.
Listen to your body more than any calendar. Pain, increased swelling, or unusual discharge are signals to slow down and check in with your care team. The goal isn’t speed – it’s a safe, full recovery that honors the significance of what your body just went through.
Schedule Your Gender-Affirming Surgery at Flourish Surgical Arts
Taking the next step toward your gender-affirming surgery is a deeply personal decision, and at Flourish Surgical Arts, you’ll never have to navigate it alone. Our team understands that the first few weeks following your procedure are critical, which is why every patient receives thorough guidance on what to expect, how to rest, and when to reach out. With each surgery performed at Flourish Surgical Arts, the care doesn’t end when you leave the operating room – our surgical team stays actively involved, monitoring healing at every stage, catching potential concerns early, and adjusting your care plan as needed. You’ll also receive guidance on building a strong support system before your procedure date, because having the right people around you during recovery makes a measurable difference in how smoothly the process goes.
If you’re ready to move forward, Flourish Surgical Arts is ready to walk alongside you – from your very first consultation to your final follow-up appointment.
Conclusion
Recovering from top surgery requires patience, preparation, and a willingness to follow your surgeon’s instructions even when you’re starting to feel better. In the early weeks, it’s essential to avoid strenuous exercise and heavy lifting, as placing strain on the upper body before tissues have properly knit together can lead to poor wound healing and, in more serious cases, complications like blood clots or fluid accumulation. Wearing a compression binder as directed helps prevent fluid buildup and supports the upper chest as your body adjusts to its new contours. This is especially important for those who have undergone double-incision procedures, in which the surgical area is more extensive. Stick to loose-fitting clothing that doesn’t rub against incisions, avoid putting pressure on healing tissue, and stay hydrated to support blood flow and cellular repair throughout the recovery period.
As healing progresses, your surgeon will clear you for increasing levels of movement – starting with light physical activity like short walks before gradually reintroducing weight-bearing exercises over several weeks. Attend all regular follow-up appointments without skipping them, as these visits allow your care team to monitor you and address any signs of complications early. Take your prescribed medications on schedule to manage pain effectively, and don’t hesitate to call your surgeon immediately if you experience severe pain, unexpected swelling, or any changes at the incision site. Ask trusted friends or family members to help with some responsibilities –cooking, driving, childcare – so you can focus entirely on rest and recovery. The more carefully you protect this window of healing, the better your long-term results will be.